Cervical cancer is a type of cancer that occurs in the cells of the cervix — the lower part of the uterus that connects to the vagina.
Various strains of the human papillomavirus (HPV), a sexually transmitted infection, play a role in causing most cervical cancer.
When exposed to HPV, the body's immune system typically prevents the virus from doing harm. In a small percentage of people, however, the virus survives for years, contributing to the process that causes some cervical cells to become cancer cells.
Causes
Where cervical cancer begins
Risk factors for cervical cancer include:
Many sexual partners. The greater your number of sexual partners — and the greater your partner's number of sexual partners — the greater your chance of acquiring HPV.
Early sexual activity. Having sex at an early age increases your risk of HPV.
Other sexually transmitted infections (STIs). Having other STIs — such as chlamydia, gonorrhea, syphilis, and HIV/AIDS — increases your risk of HPV.
A weakened immune system. You may be more likely to develop cervical cancer if your immune system is weakened by another health condition and you have HPV.
Smoking. Smoking is associated with squamous cell cervical cancer.
Symptoms
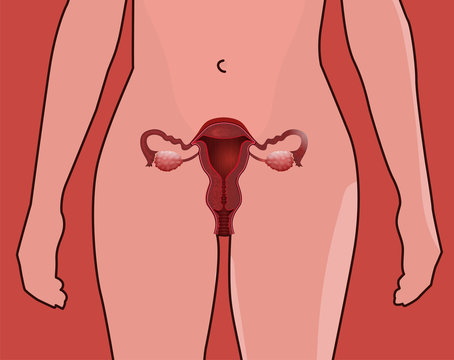
Female reproductive system
Early-stage cervical cancer generally produces no signs or symptoms.
Signs and symptoms of more-advanced cervical cancer include:
Vaginal bleeding after intercourse, between periods, or after menopause
Watery, bloody vaginal discharge that may be heavy and have a foul odor
Pelvic pain or pain during intercourse.
Diagnosis
Cone biopsy Open pop-up dialog box
If cervical cancer is suspected, your doctor is likely to start with a thorough examination of your cervix. A special magnifying instrument (colposcope) is used to check for abnormal cells.
During the colposcopic examination, your doctor is likely to take a sample of cervical cells (biopsy) for laboratory testing. To obtain tissue, your doctor may use:
Punch biopsy, which involves using a sharp tool to pinch off small samples of cervical tissue.
Endocervical curettage, which uses a small, spoon-shaped instrument (curet) or a thin brush to scrape a tis
Treatment for cervical cancer depends on several factors, such as the stage of cancer, other health problems you may have, and your preferences. Surgery, radiation, chemotherapy, or a combination of the three may be used.
Surgery
Early-stage cervical cancer is typically treated with surgery. Which operation is best for you will depend on the size of your cancer, its stage, and whether you would like to consider becoming pregnant in the future.
Options might include:
Surgery to cut away cancer only. For very small cervical cancer, it might be possible to remove cancer entirely with a cone biopsy. This procedure involves cutting away a cone-shaped piece of cervical tissue but leaving the rest of the cervix intact. This option may make it possible for you to consider becoming pregnant in the future.