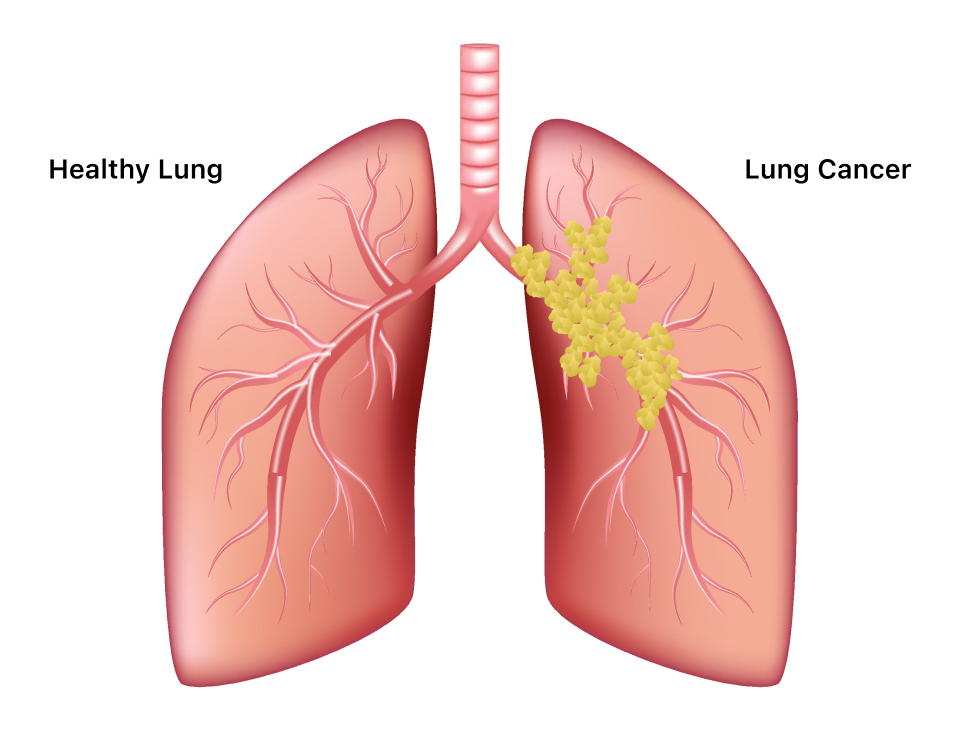
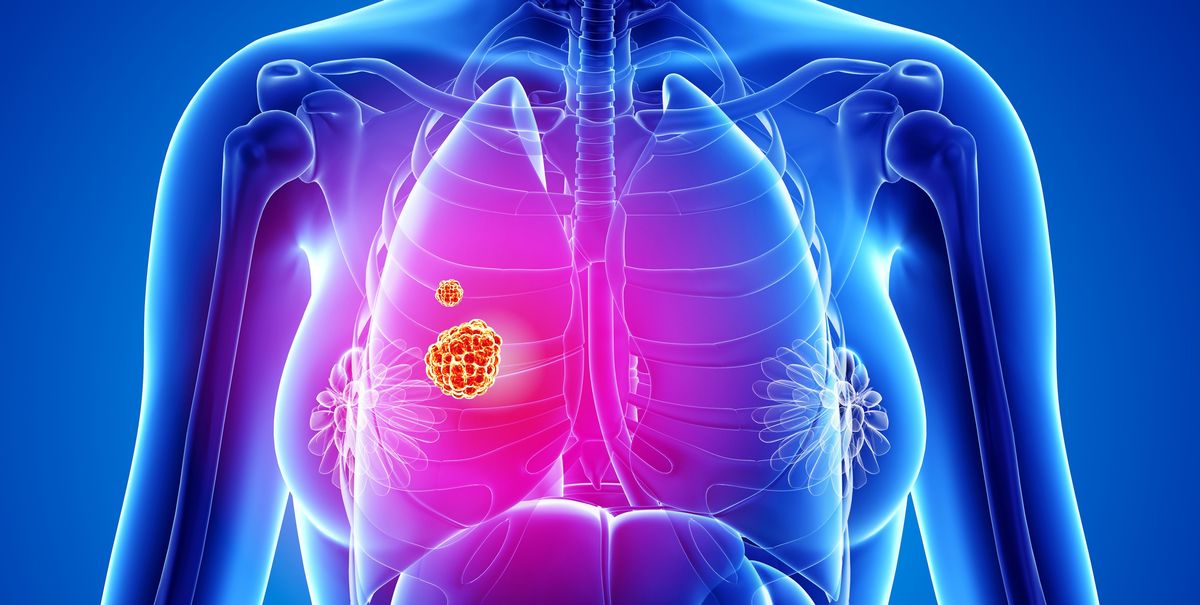
Lung cancer is a type of cancer that begins in the lungs. Your lungs are two spongy organs in your chest that take in oxygen when you inhale and release carbon dioxide when you exhale.
Lung cancer is the leading cause of cancer deaths worldwide.
People who smoke have the greatest risk of lung cancer, though lung cancer can also occur in people who have never smoked. The risk of lung cancer increases with the length of time and number of cigarettes you've smoked. If you quit smoking, even after smoking for many years, you can significantly reduce your chances of developing lung cancer.
A number of factors may increase your risk of lung cancer. Some risk factors can be controlled, for instance, by quitting smoking. And other factors can't be controlled, such as your family history.
Risk factors for lung cancer include:
Lung cancer typically doesn't cause signs and symptoms in its earliest stages. Signs and symptoms of lung cancer typically occur when the disease is advanced.
Signs and symptoms of lung cancer may include:
Make an appointment with your doctor if you have any persistent signs or symptoms that worry you.
If you smoke and have been unable to quit, make
Bronchoscopy
Testing healthy people for lung cancer
People with an increased risk of lung cancer may consider annual lung cancer screening using low-dose CT scans. Lung cancer screening is generally offered to older adults who have smoked heavily for many years or who have quit in the past 15 years.
Discuss your lung cancer risk with your doctor. Together you can decide whether lung cancer screening is right for you.
Tests to diagnose lung cancer
If there's reason to think that you may have lung cancer, your doctor can order a number of tests to look for cancerous cells and to rule out other conditions.
Tests may include:
You and your doctor choose a cancer treatment plan based on a number of factors, such as your overall health, the type and stage of your cancer, and your preferences.
In some cases, you may choose not to undergo treatment. For instance, you may feel that the side effects of treatment will outweigh the potential benefits. When that's the case, your doctor may suggest comfort care to treat only the symptoms the cancer is causing, such as pain or shortness of breath.
Lung cancer surgeryOpen pop-up dialog box
During surgery, your surgeon works to remove the lung cancer and a margin of healthy tissue. Procedures to remove lung cancer include: