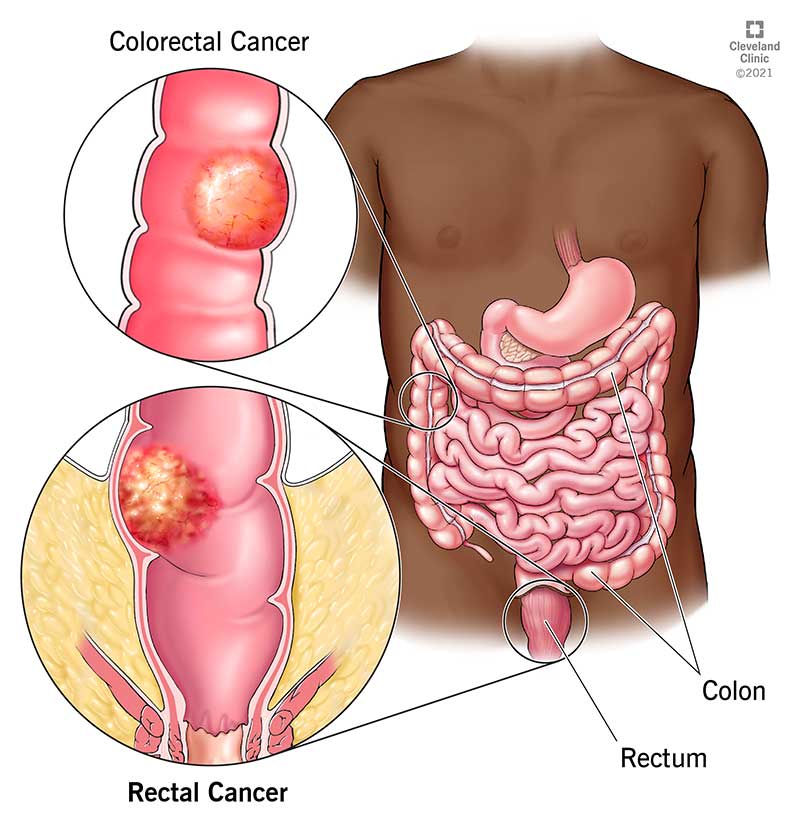
Colon cancer is a type of cancer that begins in the large intestine (colon). The colon is the final part of the digestive tract.
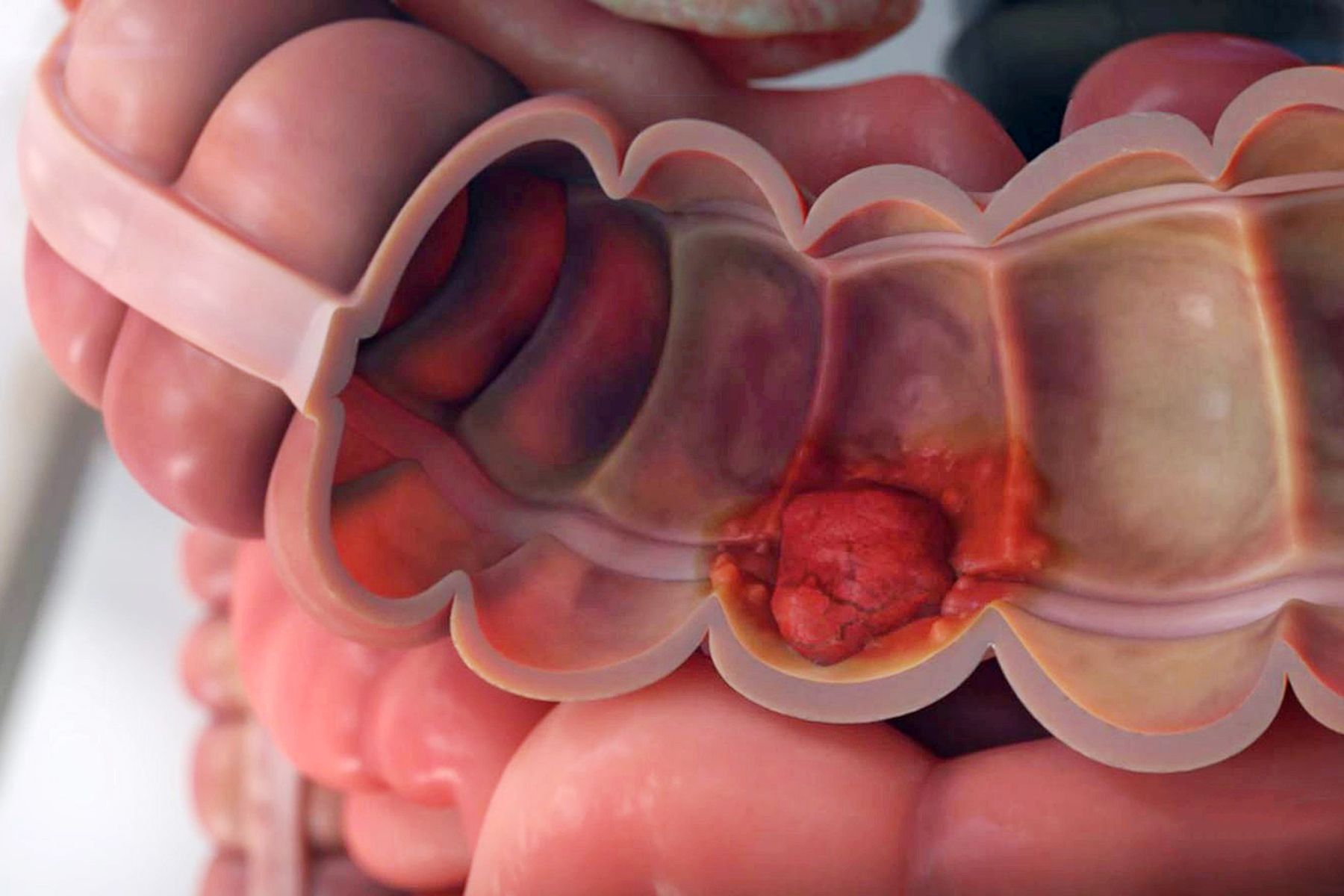
Colon cancer typically affects older adults, though it can happen at any age. It usually begins as small, noncancerous (benign) clumps of cells called polyps that form on the inside of the colon. Over time some of these polyps can become colon cancers.
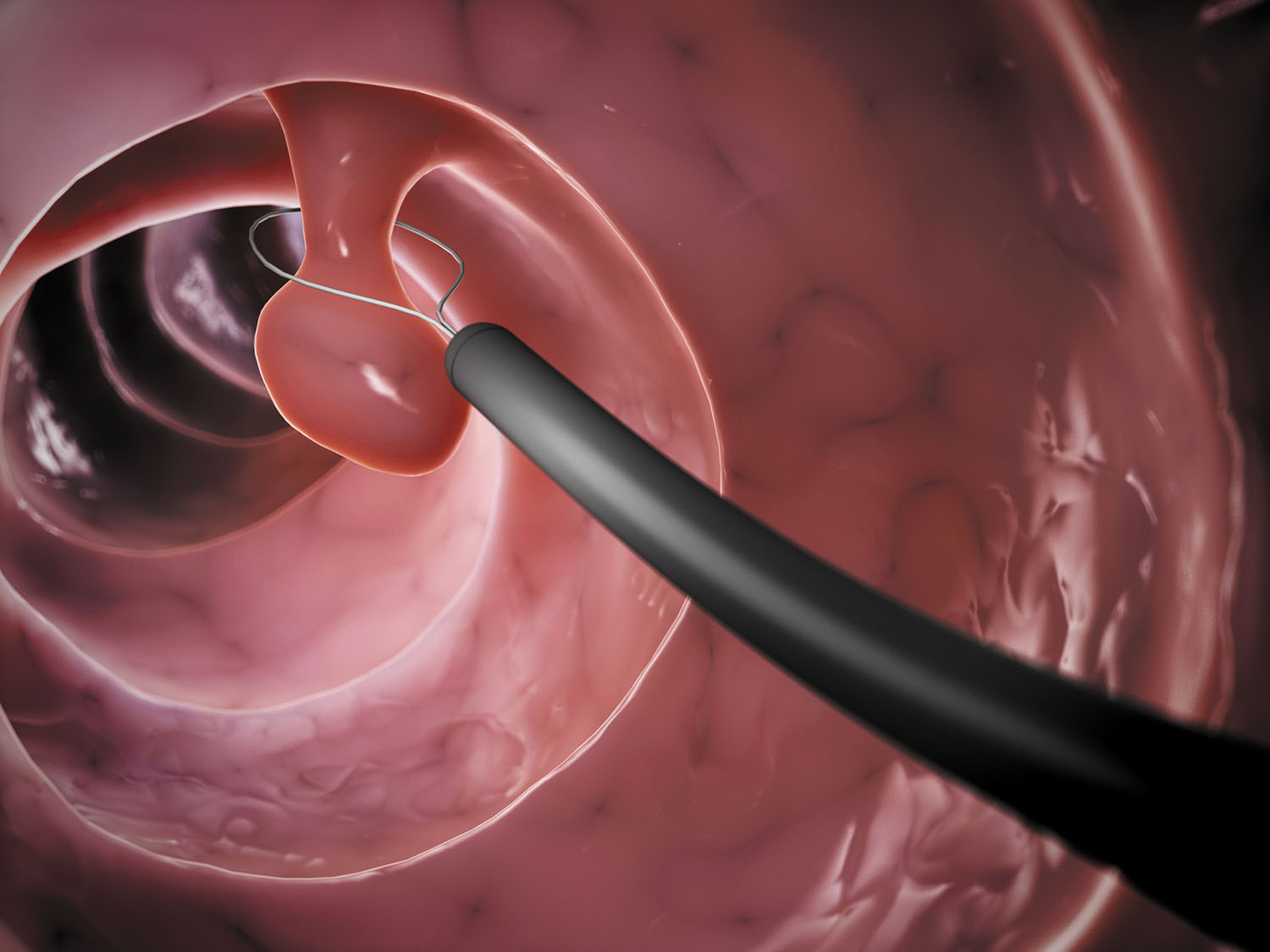
Polyps may be small and produce few, if any, symptoms. For this reason, doctors recommend regular screening tests to help prevent colon cancer by identifying and removing polyps before they turn into cancer.
If colon cancer develops, many treatments are available to help control it, including surgery, radiation therapy, and drug treatments, such as chemotherapy, targeted therapy, and immunotherapy.
Colon cancer is som
Factors that may increase your risk of colon cancer include:
Signs and symptoms of colon cancer include:
Doctors recommend certain screening tests for healthy people with no signs or symptoms in order to look for signs of colon cancer or noncancerous colon polyps. Finding colon cancer at its earliest stage provides the greatest chance for a cure. Screening has been shown to reduce your risk of dying of colon cancer.
Doctors generally recommend that people with an average risk of colon cancer begin screening around age 50. But people with an increased risk, such as those with a family history of colon cancer or African-American heritage, should consider screening sooner.
Several screening options exist — each with its own benefits and drawbacks. Talk about your options with your doctor, and together you can decide which tests are appropriate for you. If a colonoscopy is used for screening, polyps can be removed during the procedure before they turn into cancer.
Which treatments are most likely to help you depends on your particular situation, including the location of your cancer, its stage, and your other health concerns. Treatment for colon cancer usually involves surgery to remove cancer. Other treatments, such as radiation therapy and chemotherapy, might also be recommended. If your colon cancer is very small, your doctor may recommend a minimally invasive approach to surgery, such as:Treatment.
Surgery for early-stage colon cancer